On 26 March 2026, Lira University officially launched the M-CARE Project at Margaritha Hotel in Lira City, marking a major milestone in efforts to strengthen the management of chronic conditions and mental health in Uganda. The event brought together a wide range of stakeholders, including representatives from the Ministry of Health, district and city leadership, development partners, health professionals, civil society organizations, academia, community members, and the media. Uganda now joins Ghana and Kenya in implementing this five-year, multi-country initiative aimed at transforming care through integrated primary health care systems.
The launch highlighted the growing burden of non-communicable diseases and mental health conditions across Uganda and the urgent need for coordinated responses. Stakeholders emphasized that one in four Ugandans is living with hypertension, with a significant proportion unaware of their condition, while millions continue to experience mental health challenges, often in silence due to stigma. These challenges are compounded by lifestyle risk factors such as unhealthy diets, physical inactivity, and increasing rates of overweight and obesity. Despite this rising burden, health services remain fragmented, requiring patients with multiple conditions to move between different clinics with limited coordination.
In his opening remarks, Dr. Andrew Ojilong, speaking on behalf of the Vice Chancellor of Lira University, described the launch as a landmark moment for the institution and Northern Uganda. He emphasized that non-communicable diseases are placing increasing strain on households, communities, and health systems, and reaffirmed the university’s commitment to supporting evidence-based solutions to these challenges.
The Principal Investigator for Uganda, Associate Professor Benard Omech, welcomed participants and highlighted the urgent need to strengthen integrated care. He noted that many patients with multiple conditions are forced to navigate a fragmented system that does not adequately respond to their needs. Using a practical example, he illustrated the reality faced by patients managing hypertension, diabetes, and depression across different clinics, stating, “One patient, many clinics, no system.” He emphasized that the M-CARE Project seeks to address this gap by promoting coordinated, patient-centred care within the primary health care system.
Delivering the keynote address, Dr. Charles Oyoo Akiya, Commissioner for Non-Communicable Diseases at the Ministry of Health, described the launch as a defining moment for Uganda’s health system. He warned that the country is undergoing a “silent but dangerous transition,” with non-communicable diseases and mental health conditions increasingly affecting individuals, families, and communities. He called for urgent action, emphasizing the need to move “from fragmented efforts to integrated care, and from policy commitments to real, measurable improvements in people’s lives.” He further stressed that diseases do not occur in isolation and therefore should not be treated in isolation, highlighting the importance of integrated, people-centred approaches.
The M-CARE Project aims to integrate the management of hypertension, diabetes, and depression at the primary health care level. In Uganda, the project will be implemented across 60 health facilities in Lira, Oyam, Kole districts, and Lira City. By building on existing World Health Organization frameworks, including the Package of Essential Noncommunicable Disease Interventions and the Mental Health Gap Action Programme, the initiative seeks to strengthen service delivery, improve patient outcomes, and enhance the efficiency of the health system.
Updates presented during the launch showed that significant progress has already been made since the project began in July 2025. These include the establishment of project offices, recruitment of staff, creation of governance structures, stakeholder engagement at national and district levels, and the mapping of 76 health facilities across the Lango sub-region. The findings from this mapping exercise revealed important gaps, including limited training in integrated care approaches, weak referral systems, shortages of essential medicines, and limited digital infrastructure for patient tracking and follow-up. These findings reinforced the need for targeted investments in strengthening primary health care systems.
Mental health emerged as a central theme throughout the discussions. Participants highlighted that mental health remains highly stigmatized and often misunderstood, with many individuals seeking care outside formal health systems, including through religious or traditional channels. There was strong consensus on the need to integrate mental health services into primary health care, strengthen community awareness, and engage religious and cultural leaders as part of the solution. Stakeholders also emphasized the importance of training frontline health workers and community health teams to improve early detection and referral of mental health conditions.
The launch also featured a policy panel discussion, where stakeholders reflected on practical ways to improve service delivery. Participants strongly supported integrated care approaches, noting that a one-stop model would improve efficiency, reduce patient burden, and enhance quality of care. One participant noted that “integration creates efficiency and improves patient care,” while others emphasized that better coordination of services would significantly improve patient experiences. The discussions also included personal reflections on lifestyle risk factors, reinforcing the importance of promoting healthier behaviours within communities.
Several key challenges were identified during the launch, including health worker shortages, medicine stock-outs, weak referral systems, limited digital health infrastructure, and low community awareness. Despite these challenges, stakeholders expressed optimism that coordinated efforts, strengthened partnerships, and targeted investments can address these gaps. Recommendations included scaling up training in integrated care approaches, strengthening community engagement, improving referral and follow-up systems, and investing in digital health solutions.
The event concluded with the official launch ceremony led by national and local leaders, during which stakeholders signed a Commitment Charter to demonstrate their collective resolve to support the implementation of the M-CARE Project in Uganda. This symbolic act underscored a shared commitment to moving beyond fragmented care towards a more coordinated, patient-centred, and evidence-based health system.
The M-CARE Project represents more than a research initiative; it marks the beginning of a transformative journey toward improving how health care is delivered and experienced in Uganda. With strong leadership, broad stakeholder engagement, and a clear vision for integrated care, the project is well-positioned to strengthen health systems and improve outcomes for individuals living with chronic conditions and mental health challenges across the country and the wider region.
 Dr. Maxso presents on the progress of M-CARE project since inception in July 2025 to date
Dr. Maxso presents on the progress of M-CARE project since inception in July 2025 to date

Official Launch of the M-CARE Project
The official launch was presided over by the Mayor Lira City and the Guest of Honour, Commissioner National NCD, MoH who commended the consortium for prioritizing chronic care and mental health.

The M-Care and Lira University Leadership proudly present the signed commitments Charter by all stakeholders during the project launch
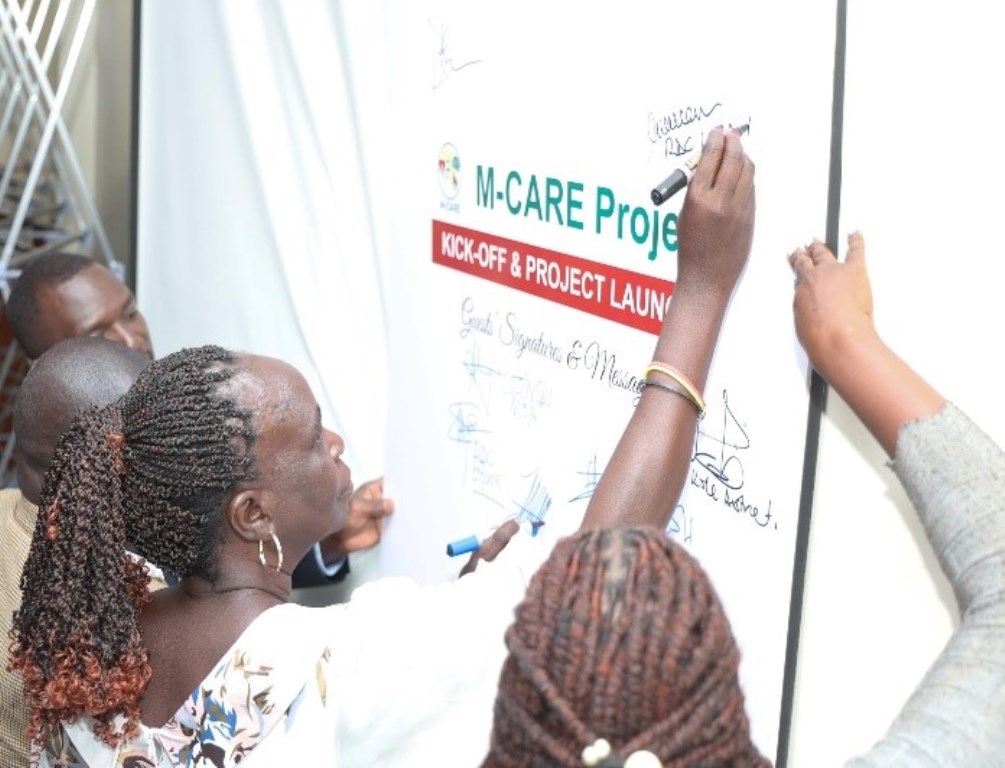
The RDC Lira District appends her signature during the M-CARE project launch.

The Panelists comprised diverse categories of stakeholders of the M-CARE project

Participants took a physical exercise break
updating page …




